This will only be perfomed if the request meets the current selection critera in the Trust Guidelines
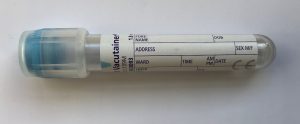
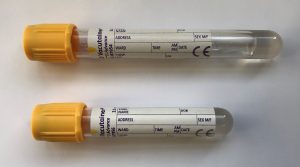
Peripheral blood – 3 x Sodium citrate and & 1 x serum
Heritable thrombophilia describes an inherited tendency to develop venous thrombosis (DVT and/or PE)1. Deficiencies of the naturally occurring anticoagulants Antithrombin, Protein C and Protein S have been linked with familial venous thrombosis.
Some tests for heritable thrombophilia (assays of Antithrombin, Protein C and Protein S) are affected by the acute post-thrombotic state and by anticoagulant use. Consequently, thrombophilia testing should be delayed until at least 6 weeks after cessation of anticoagulant therapy as discussed with a Consultant Haematologist. Thrombophilia testing should be avoided during pregnancy and in patients using combined oral contraceptives or hormone replacement therapy.
Which patients should be considered for thrombophilia testing?
Thrombophilia results are often difficult to interpret and can be misleading. Please use the contact numbers below to discuss, or consider referring the patient to the haematology clinic if appropriate.
(A) Patients with symptoms of thrombophiliaPlease note: Testing for heritable thrombophilia is NOT indicated in UNSELECTED patients presenting with venous thrombosis.
It is recommended that thrombophilia screening should be undertaken in the following patients:
(B) First degree relatives WITHOUT symptoms of thrombophilia
Testing asymptomatic first degree adult relatives (siblings, parents, offspring if ≥16 years) of patients with a history of venous thrombosis may be indicated in some circumstances. Identification of family members at risk for venous thrombosis may provide the opportunity for short-term targeted thrombophylaxis in periods of increased thrombotic risk (eg. surgery, trauma or immobilization).
The testing of asymptomatic relatives of patients with low risk thrombophilia (such as factor V Leiden or prothrombin gene variants) is NOT indicated.
The testing of asymptomatic relatives of patients with high risk thrombophilia (deficiency of Antithrombin, Protein C or Protein S) should only be considered in selected thrombosis-prone families. Please discuss with a Consultant Haematologist before taking samples.
The absence of a proven heritable risk factor reduces the utility of thrombophilia testing and wherever possible the affected family member(s) should be tested first. If this is not possible, a negative result in the asymptomatic relative should be interpreted with caution since it does not exclude an increased risk of venous thrombosis.
Please send 3 coagulation tubes (blue topped bottles) requesting a ‘Thrombophilia Screen’ to the haematology laboratory. We aim to provide a customised clinical / laboratory report for every thrombophilia screen, so full clinical details are essential. Samples with insufficient clinical details or those that do not meet guidelines for testing will be stored for one month, to allow time for the requestor to supply further information or discuss the request with a Consultant Haematologist.
In addition a clotted blood Brown top is required for anticardiolipin assay.
If you have any questions about heritable risk factors for thrombophilia please contact
Table 1. Frequency of thrombophilia and relative risk estimates for various clinical manifestations.3
| Antithrombin Deficiency | Protein C Deficiency | Protein S Deficiency | Factor V Leiden variant | Prothrombin variant | |
| Prevalence in general population | 0.02% | 0.2% | 0.03-0.13% | 3-7% | 0.7-4% |
| Relative risk for 1st venous thrombosis | 5-10 | 4-6.5 | 1-10 | 3-5 | 2-3 |
| Relative risk for recurrent venous thrombosis | 1.9-2.6 | 1.4-1.8 | 1.0-1.4 | 1.4 | 1.4 |
| Relative risk for arterial thrombosis | No association | No consistent association | No consistent association | 1.3 | 0.9 |
| Relative risk for pregnancy complications | 1.3-3.6 | 1.3-3.6 | 1.3-3.6 | 1.0-2.6 | 1.1-1.2 |
Protein C 70-140 %
Protein S 53 – 109%
Antithrombin 80 – 120 iu/dl
Lupus anticoagulant not applicable
Up to 3 weeks
In house for coagulation based tests.
Factor V Leiden and Prothrombin Gene mutations are no longer routinely available. If molecular investigation are required, please discuss with a Consultant Haematologist who will advise on testing.
Clinical advice is available from the Haematology Medical team (contact RD&E switchboard on 01392 411611)
Specimen Labelling Procedure